The Ultimate Guide to Leg Health: How to Prevent and Treat Varicose Veins
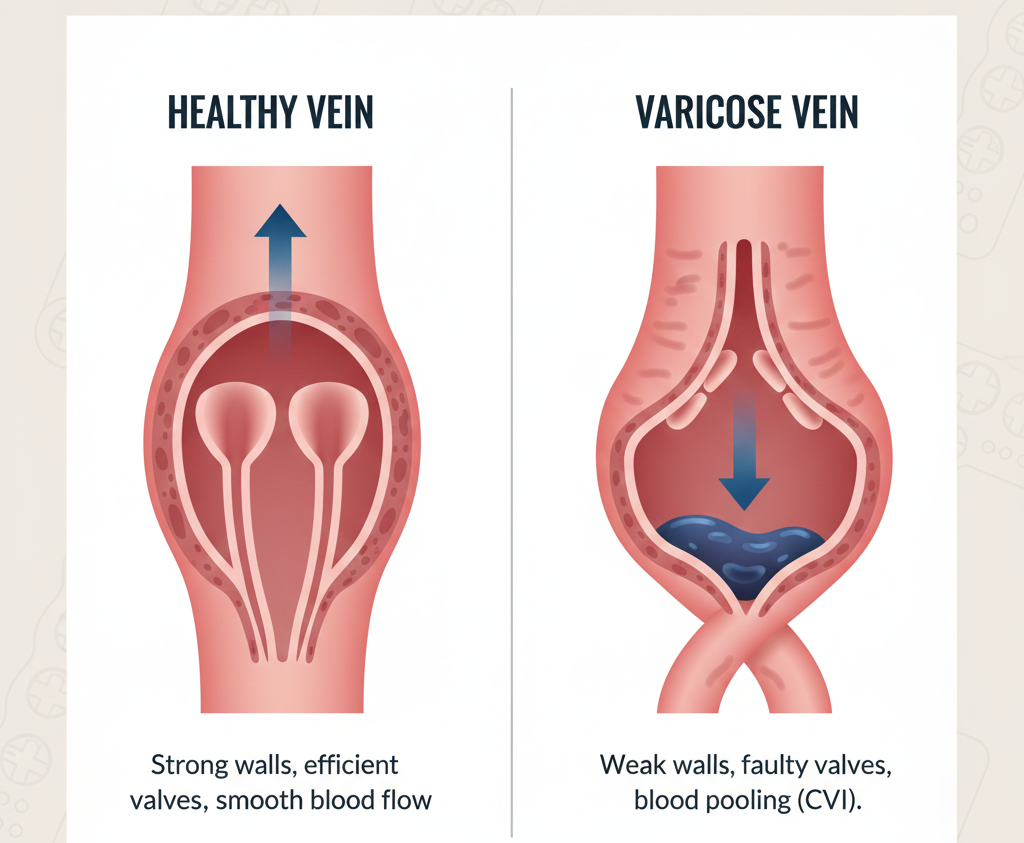
For many, the appearance of bulging, bluish veins on the legs is seen merely as an inevitable sign of aging or a cosmetic nuisance. However, medically speaking, varicose veins are the most visible and often painful symptom of a deeper condition known as Chronic Venous Insufficiency (CVI).
In this exhaustive guide, we will explore the biological mechanisms behind venous health, the hidden risk factors, and the multi-layered approach required to prevent, manage, and treat this condition effectively.
1. Understanding the Science: What Are Varicose Veins?
Varicose veins are not just “thick veins.” They are permanent dilations of the veins characterized by a loss of elasticity and the failure of internal valves. While they can manifest in various parts of the body (such as the esophagus or the pelvic area), they are overwhelmingly most frequent in the lower extremities.
The Circulatory Battle Against Gravity
To understand why they form, we must look at how our blood moves. The circulatory system uses two main “highways”:
- Arteries: These act as the outbound route, carrying oxygenated blood from the heart to the rest of the body.
- Veins: These are the return route. Unlike arteries, veins in the legs must fight against gravity to push blood upward toward the heart.
To achieve this “uphill” climb, our veins are equipped with one-way valves. These valves open to let blood through and snap shut to prevent it from flowing backward. When these valves weaken or the vein walls stretch (becoming “incompetent”), blood begins to pool in the legs. This is the physiological birth of Chronic Venous Insufficiency (CVI).
2. Who is at Risk? The Determining Factors
While anyone can develop CVI, certain demographics and lifestyle choices act as catalysts for the condition.
The Gender and Hormone Connection
Statistically, women are significantly more likely to develop varicose veins than men. This is largely due to progesterone, a hormone that relaxes vein walls. Life stages involving high hormonal shifts—such as puberty, menopause, and especially pregnancy—increase the risk of venous dilation.
The Role of Genetics and Age
Vascular health is heavily hereditary. if both your parents had varicose veins, your chances of developing them are close to 90%. Furthermore, as we age (typically between 30 and 70 years old), the elastic fibers in our veins naturally degrade, making the vessels more prone to stretching.
The Impact of Pregnancy
Pregnancy is a “perfect storm” for venous issues. During this time:
- Hormones loosen the vein walls to accommodate increased blood volume.
- Blood Volume increases by up to 50% to support the fetus.
- Physical Pressure: As the uterus grows, it compresses the pelvic veins, making it harder for blood to drain from the legs.Research shows that 40% of pregnant women experience symptoms of CVI, often starting around the third month and peaking in the sixth.
3. Lifestyle: The Modern Enemy of Circulation
Two of the biggest contributors to CVI in the 21st century are obesity and postural habits.
- Weight Management: Excess body weight acts as a literal “clog” for the vascular system. It increases the pressure within the venous system, causing the valves to wear out prematurely.
- The Postural Factor: Our bodies were designed to move. Spending 8 hours a day standing (like teachers or pharmacists) or sitting with legs crossed (office workers) creates “venous stasis”—a state where blood flow becomes sluggish and stagnant.
4. The Psychological and Emotional Toll
We often underestimate the impact of CVI on mental health. It isn’t just about pain; it’s about confidence.
According to the II CinfaSalud Study, the emotional weight of varicose veins is profound:
- 28% of women report feeling ashamed to show their legs in public (avoiding skirts or swimming pools).
- 21% of patients claim the condition has directly lowered their self-esteem.
Recognizing CVI as a medical condition rather than a “flaw” is the first step toward seeking treatment and regaining confidence.
5. Prevention: Proactive Habits for Healthy Veins
You cannot change your DNA, but you can change your veins’ environment. Here is a blueprint for prevention:
Movement is Medicine
Incorporate “vascular gymnastics” into your day. If you work at a desk, do ankle circles or heel-toe lifts every hour. Low-impact exercises like walking, swimming, and cycling are ideal because they engage the calf muscle pump—often called the “second heart”—which helps push blood upward.
Temperature Control
Heat is a vasodilator (it opens veins). Avoid prolonged hot baths, saunas, or direct sun exposure on your legs. Conversely, cold water rinses at the end of a shower can help constrict veins and improve tone.
Nutrition and Hydration
A diet high in fiber prevents constipation, which is a hidden cause of increased abdominal pressure that affects leg veins. Antioxidant-rich foods (berries, citrus, leafy greens) protect the integrity of the vascular lining.
6. Treatment Modalities: From Conservative to Surgical
If prevention isn’t enough, modern medicine offers a spectrum of solutions tailored to the severity of the case.
A. Conservative Treatments
- Compression Therapy: This is the most effective non-invasive treatment. Compression stockings apply graduated pressure (tightest at the ankle, loosening as they go up) to assist the valves.
- Phlebotonics: These are medications (capsules) or topical gels that improve the tone of the vein walls and reduce inflammation.
B. Minimally Invasive & Surgical Techniques
When veins become too damaged, they may need to be “closed” or removed to allow blood to divert to healthy veins.
| Technique | Description | Best For |
| Sclerotherapy | Injecting a chemical foam that scars and closes the vein. | Small to medium veins (spider veins). |
| Endovenous Laser/Radiofrequency | Using heat via a catheter to collapse the vein from the inside. | Large internal veins (Saphenous). |
| Safenectomy (Stripping) | The traditional surgical removal of the diseased vein. | Severe, advanced cases of CVI. |
| CHIVA Strategy | A hemodynamic approach that redirects blood flow without removing the vein. | Patients wanting a conservative surgical option. |
7. Summary and Final Recommendations
Managing varicose veins is a marathon, not a sprint. While surgical options are highly effective, they do not “cure” the underlying tendency for CVI. Therefore, the most successful patients are those who combine medical intervention with lifelong habits: movement, weight control, and compression.
If you begin to feel “heavy legs,” nighttime cramping, or see small “spider” clusters, consult a vascular specialist (angiologist). Early intervention is the key to preventing skin ulcers, blood clots, and permanent swelling.